Clinical efficacy of digital flexible ureteroscopy for renal stone management and postoperative quality of life for the treatment of lower pole stones: a single-center, non-randomized study
Flexible ureteroscopy in renal stone management
- Received:
- August 4, 2025
- Accepted:
- September 5, 2025
- Published Online:
- September 19, 2025
- Printed:
- October 1, 2025
Authors
Abstract
AimThis study aimed to evaluate the safety and efficacy of digital flexible ureteroscopy in the management of lower pole stones and to assess patients’
postoperative quality of life.
MethodsA longitudinal, single-center, nonrandomized cohort study was conducted on patients with renal calculi eligible for flexible ureteroscopy. The study population comprised 44 patients diagnosed with treatment of lower pole stones who underwent treatment at Bach Mai Hospital between January 2023 and October 2024. Surgical outcomes, including surgery duration, stone-free rate, duration of hospitalization, surgical complications, and quality of life, were evaluated and monitored during the follow-up period.
ResultsThe mean age of the patients was 51.4 years, and the mean stone size was 13.7 mm. Immediately postoperative stone-free rates were 79.5 %, 77.3 % at 1-month, and 68.2 % at 3-month. The mean operative time was 73.4 minutes, the lithotripsy duration was 55.7 minutes, and the average hospital stay was 5.7 days. Only 1 minor complication (2.3%) was recorded. The quality-of-life scores significantly improved over time (p < 0.001), with most patients reporting no disruption to daily activities after 1 month.
ConclusionSingle-use digital flexible ureteroscopy is a safe and effective modality for managing lower-pole renal stones, offering high stone-free rates, low complication rates, and significant improvements in patient quality of life. Further large-scale, controlled studies are needed to confirm these findings and evaluate long-term outcomes.
Keywords
Introduction
Renal calculi represent one of the most prevalent urological conditions. Globally, the prevalence is notably high, with reported rates ranging from 7 to 13% in North America, 5–9% in Europe, and approximately 1–5% in Asia 1. The prevalence of urinary stones in Vietnam ranges from 2% to 12%, and approximately 40% of cases are renal calculi 2. This elevated incidence is potentially associated with dehydration due to high ambient temperatures during the summer months, resulting in reduced urine output 3. With the ongoing rise in global temperatures attributable to climate change, projections suggest that the number of individuals affected by urinary stones could increase from 1.6 to 2.2 million by the year 2050 4. If renal calculi are not appropriately managed, the patient may experience severe complications, including pyelonephritis, interstitial nephritis, hydronephrosis, pyonephrosis, anuria, oliguria, and both acute and chronic renal failure 5.
Currently, a variety of treatment modalities for upper urinary tract stones are being implemented in Vietnam and all over the globe. The adoption of flexible endoscopes has gained momentum because of their demonstrated efficacy and safety profiles 6. In recent decades, there have been substantial advancements in both the technology and clinical application of minimally invasive procedures within the field of urology. Flexible ureteroscopy has evolved to become a widely used diagnostic and therapeutic tool for many upper urinary tract pathologies. The most common indication for ureteroscopy is treatment of upper urinary tract stones with the aid of holmium, mainly Yttrium Aluminum Garnet (YAG) laser lithotripsy. This technique is recognized for its high efficacy and favorable safety profile, with relatively few complications. However, the effectiveness of lithotripsy for lower pole stones remains suboptimal due to the anatomical constraints of the lower calyx. Several studies have indicated that the infundibulopelvic angle (IPA) plays a critical role in determining the success of flexible ureteroscopy (FURS) combined with holmium laser lithotripsy 7. A systematic review of the literature reported that an acute IPA (<30°) is significantly associated with lower success rates, particularly when accompanied by prolonged operative time or larger stone size. In contrast, factors such as the use of a ureteral access sheath, infundibular width (IW), and infundibular length (IL) were not found to significantly impact treatment outcomes 8. Ongoing innovations in flexible ureteroscopic technology have further expanded its clinical utility, positioning it as a first-line treatment option in the management of urolithiasis 9. In addition, the use of flexible endoscopes may alleviate hand fatigue experienced by surgeons during prolonged procedures, as it eliminates the need for continuous manual deflection control, which is beneficial when managing calculi located in the lower pole calyx 11. To address these limitations, flexible endoscopes have been developed as an alternative to conventional reusable models. Numerous studies have demonstrated their high efficacy in the treatment of urolithiasis 10,12,13.
In many regions, including Vietnam, the management of renal calculi remains suboptimal due to limited access to advanced endourological techniques, delayed diagnosis, and inconsistent follow-up. However, to date, there has been no comprehensive and systematic investigation specifically addressing the use of digital flexible ureteroscopy for the treatment of urinary stones, particularly lower pole stones, and post-treatment patient monitoring. Accordingly, the present study aims to evaluate the safety and efficacy of digital flexible ureteroscopy in the management of renal calculi with lower pole stones and to assess patients’ postoperative quality of life.
Materials and Methods
Study Participants
This study was designed as a single-center, non-randomized study. The study population comprised 44 patients diagnosed with lower pole renal calculi who underwent treatment at Bach Mai Hospital between January 2023 and October 2024.
We defined patients with lower pole renal calculi as those with stones located in calyces arising from the lower third of the renal collecting system, as determined by preoperative imaging (non-contrast CT or ultrasound). The exclusion criteria were urinary tract obstructions (e.g., urethral or ureteral strictures, ureteropelvic junction obstruction, Grade 4 hydronephrosis), non-functioning kidneys, pregnancy, age under 16, congenital renal anomalies (e.g., duplex or horseshoe kidney), and significant spinal deformities.
A total of 240 patients underwent endoscopic treatment for urolithiasis at the Nephrology Department of Bach Mai Hospital between 2023 and 2024; we excluded 23 subjects who declined to participate in the study. We also excluded 43 patients who were lost in the follow-up period, and 30 patients were removed because their stones were not located in the lower pole of the kidney. Data for 44 subjects were analyzed in this study (Figure 1).
Clinical Characteristics
The following clinical variables were recorded at the time of patient evaluation: age, sex, body mass index (BMI), prior history of treatment on the affected kidney, and reason for hospital admission. Comorbid conditions, including hypertension, diabetes mellitus, or other endocrine disorders, were also documented. BMI is calculated as weight in kilograms divided by the square of the height in meters (kg/m2) and is categorized into four groups according to the Asian-Pacific cutoff points 14.
Ultrasound Assessment
All patients underwent renal ultrasonography to assess stone size, location, and the degree of hydronephrosis. Stone size was measured by maximum length, and the location was classified as upper, middle, or lower calyx.
Technical Procedure
All procedures were performed under general anesthesia with the patient in the lithotomy position, consistent with conventional retrograde ureteroscopy. A C-arm fluoroscopy unit was positioned to allow for continuous imaging from the bladder to the renal pelvis. A 6 Fr JJ stent (Marflow, Switzerland) was placed 7–14 days before facilitating passive ureteral dilation. In the absence of prior stenting, ureteral dilation was achieved intraoperatively using a semi-rigid ureteroscope, followed by JJ stent placement.
A cystoscope was introduced to retrieve the distal end of the JJ stent, and a guidewire was advanced through the stent into the renal pelvis under C-arm guidance. For cases involving ureteral, renal pelvic, or upper calyceal stones, a semi-rigid ureteroscope was advanced along the guidewire for initial lithotripsy; subsequently, it was withdrawn, leaving the guidewire in place. A 12–14 Fr ureteral access sheath (Navigator HD™, Boston Scientific, USA) was then introduced over the guidewire into the renal pelvis under C-arm control. Afterwards, the guidewire and obturator were removed. A single-use digital flexible ureteroscope (Uscope UE3022™, Pusen Medical Technology Co., Zhuhai, China) was inserted through the sheath to access the collecting system, guided by both direct vision and fluoroscopy, with continuous irrigation using normal saline. The ureteroscope had an outer shaft diameter of 9.2 Fr, a lens tip diameter of 9.5 Fr (ø2.8 mm), a 3.6 Fr working channel, 270° dual deflection, and a working length of 650 mm.
This single-use flexible ureteroscope was inserted through the sheath to access the collecting system, guided by both direct vision and fluoroscopy, with continuous irrigation using normal saline. When the ureter was adequately dilated, the flexible ureteroscope could be introduced directly over the guidewire. Stones were identified, measured, and repositioned if necessary—particularly from the lower to the upper calyx or renal pelvis—to minimize scope deflection. Lithotripsy was performed using a 230 µm holmium, for which a YAG laser fiber was introduced through the ureteroscope’s working channel via a protective sheath. Stone clearance was assessed intraoperatively using both direct endoscopic visualization and fluoroscopy. Patients were considered stone-free if no residual fragments >4 mm were detected. Small residual fragments (≤4 mm) were measured based on their largest diameter and included in postoperative stone size calculations, which explains the occasional median values slightly above 4 mm despite meeting stone-free criteria. A JJ stent was placed at the end of the procedure to ensure adequate drainage.
Treatment Outcomes
-Postoperative assessment and follow-up
The procedure was considered successful when only fine gravel or stone fragments measuring ≤4 mm remained in situ or when no residual stones were visualized on intraoperative C-arm fluoroscopy 15. Stone-free status was assessed at 1 month and 3 months postoperatively using either plain abdominal radiography or renal ultrasonography. Patients were considered stone-free if no radiopaque shadows were detected at the site of the preoperative renal stone (in cases of radiopaque stones) or if any residual stone fragment or cluster had a maximal diameter of ≤4 mm.
-Complication assessment
Complications were recorded throughout the perioperative and follow-up periods. All were classified according to the Clavien–Dindo classification system, a standardized surgical complication grading system revised in 2004 by Dindo and Clavien based on their earlier 1994 proposal 16.
-Quality of life assessment
The EQ-5D-5L instrument was used to assess quality of life at admission, immediately after surgery, and postoperatively (1-month and 3-month follow-up). The EQ-5D-5L instrument comprises a descriptive system and a visual analog scale 17.
Statistical Analysis
The basic characteristics of the participants are shown according total number of patients. Continuous variables were reported as means ± standard deviation (SD), and comparisons of mean values were made using Student’s t-test. Categorical variables were expressed as numbers (percentages, %), and comparisons of proportions were made using the chi-square test. A paired t-test was used to compare the mean values, and McNemar’s test was used to compare proportions and calculate the p-values with variables that had 2-time follow- ups. Repeated measurement analysis was used to compare the mean and calculated p-values with variables from 3-time follow-ups. Statistical analyses were performed using SPSS (IBM Corporation, US) version 29.0 for Mac. All statistical tests were based on two-sided probabilities, and a p-value <0.05 is considered significant.
Ethical Approval
This study was approved by the Ethics Committee of the Institutional Review Board of Hanoi Medical University (Date: 2023-07-13, No: 876/GCN-HĐĐĐNCYSH-ĐHYHN).
Results
Patient Characteristics
The characteristics of the study population are presented in Table 1. The mean age of the participants was 51.4 years. The overall mean body mass index (BMI) was 22.4 kg/m2. The median stone size was 13.7 mm. The number of stones detected did not differ significantly between the sexes. Preoperative hematuria was reported in four patients (9.1%). A history of hypertension and diabetes was recorded in seven and five patients, respectively.
Surgical and Follow-Up Outcomes
The surgical outcomes are presented in Table 2. The mean operative time was 73.4 minutes. The average lithotripsy time was 55.7 minutes. The mean postoperative hospital duration was 6.2 days. The overall stone-free rate immediately after surgery was 79.5%. There was one recorded intraoperative complication (2.3%).
The median size of the largest stone decreased over time, being 4.5 ± 0.7 mm immediately after surgery, 2.2 ± 0.6 mm at the 1-month follow-up mark, and 1.1 ± 0.4 mm at the 3-month follow-up mark (p < 0.001). The stone-free rate improved from 77.3% at 1 month to 68.2 % at 3 months (p = 0.289). Additionally, the mean post-operative quality of life score increased significantly over the follow-up period (p < 0.001), with most patients reporting no disruption to daily activities after 1 month.
Discussion
The findings of this study demonstrate that single-use flexible ureteroscopy is a highly effective modality for the management of lower-pole stones. This minimally invasive approach not only achieves a high rate of stone clearance but also contributes to significant improvements in patients’ postoperative quality of life. These results support the growing role of flexible ureteroscopy as a safe and efficient method in the treatment of lower-pole stones.
The average lithotripsy time was 55.6 ± 27.4 minutes. The lithotripsy time in our study was similar to that reported in some other studies 13. A study by José A. Salvadó et al. (2018) reported an average lithotripsy time of 56.6 ± 38.0 minutes 18. Another study, conducted by Qiang Jing et al. (2024), reported an average lithotripsy time of 51.27 ± 13.8 minutes 19. Qinghua He et al. (2024) recorded a longer lithotripsy time, averaging about 72.4 ± 14.4 minutes 20. These differences in lithotripsy time may be due to the complexity of the stones or the difficulty of performing the procedure in each study.
In our study, the average hospital stay was 5.7 days (Table 2). This is comparable to findings from other studies utilizing minimally invasive techniques. Huayu Gao et al. (2019) reported a mean hospital stay of 4.33 ± 1.55 days following digital endoscopic lithotripsy, while Qinghua He et al. (2024) observed a duration of approximately 3.9 ± 1.2 days. When comparing different minimally invasive approaches, both Gao and He noted that the hospital stay after digital endoscopic stone removal was shorter than that observed after percutaneous nephrolithotomy (PCNL) 20,21. Although flexible ureteroscopy is associated with short hospital stays in many international settings, the mean postoperative hospitalization duration in our study was influenced by local clinical protocols, which favor extended inpatient observation even in the absence of complications. This practice may differ from global trends prioritizing early discharge.
In the present study, the overall postoperative stone-free rate (SFR) was 79.2% (Table 2). These findings are consistent with those reported in the international literature. El-Nahas et al. reported an SFR of 86.5% following flexible ureteroscopy (f-URS) for the treatment of 10–20 mm lower pole stones 22. Similarly, Gao et al. (2019) reported a postoperative SFR of 78.2% at three days in a cohort of 100 patients treated with digital endoscopic lithotripsy 20. The overall postoperative stone-free rate (SFR) was 70.5% after 3 months of follow-up. He et al. (2024) also recorded a 3-month stone-free rate of 71.5% 21.
In our study, only one minor complication (surgical fever) was recorded during the follow-up period, further supporting the idea of the procedure being minimally invasive in nature. In comparison, other studies have reported slightly higher complication rates. For example, José A. Salva et al. (2018) noted two complications following f-URS: surgical fever and hematuria 18. In a study by Huayu Gao et al. (2019), complications included fever in 23.6% of cases, abdominal pain in 7.3% of cases, and urinary tract infection in 3.6% of cases 21. Additionally, in their study, Fankhauser et al. (2021) reported that Clavien–Dindo Grade 2 complications occurred in approximately 5% of patients undergoing ureteroscopy 23. These differences may reflect differences in patient populations, surgical techniques, or perioperative management protocols. Complications were minimal in this study, further supporting the favorable safety profile of digital flexible ureteroscopy.
To our knowledge, there are relatively few studies that comprehensively assess patients’ quality of life following laparoscopic lithotripsy. One such study reported significantly greater improvements in quality-of-life scores with digital flexible ureteroscopy compared to minimally invasive percutaneous nephrolithotomy 23. In the present study, we assessed the patient-reported quality of life four times: preoperatively, immediately postoperatively, and at 1 and 3 months postoperatively. The results revealed a consistent improvement in quality-of-life scores over time, with most patients reporting minimal disruption to daily activities by the 1-month follow-up.
Limitations
Several limitations should be acknowledged. The non- randomized, single-center study design limits the ability to establish causality or control for confounding factors. Additionally, the relatively small sample size may reduce the generalizability of the findings. Finally, the analysis did not fully address risk factors associated with postoperative complications, indicating the need for further investigation to improve clinical outcomes and guide patient selection. Future studies should consider employing randomized controlled trial designs and involving multiple centers to enhance the external validity and robustness of findings.
Conclusion
The findings of this study indicate that flexible ureteroscopy is a promising and effective modality for the management of lower-pole renal stones, demonstrating a high stone-free rate and notable improvements in patient-reported quality of life. Future studies should include larger sample sizes, comparative evidence-based study designs, and longer follow-up periods to generate more robust and generalizable conclusions that could inform clinical practice.
Declarations
Ethics Declarations
This study was approved by the Ethics Committee of Institutional Review Board of Hanoi Medical University (Date: 2023-07-13, No: 876/GCN-HĐĐĐNCYSHĐHYHN)
Animal and Human Rights Statement
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Data Availability
The datasets used and/or analyzed during the current study are not publicly available due to patient privacy reasons but are available from the corresponding author on reasonable request.
Conflict of Interest
The authors declare that there is no conflict of interest.
Funding
None.
Scientific Responsibility Statement
The authors declare that they are responsible for the article’s scientific content, including study design, data collection, analysis and interpretation, writing, and some of the main line, or all of the preparation and scientific review of the contents, and approval of the final version of the article.
References
-
Sorokin I, Mamoulakis C, Miyazawa K, Rodgers A, Talati J, Lotan Y. Epidemiology of stone disease across the world. World J Urol. 2017;35(9):1301-20.
-
Nguyen LD, Nguyen TT, Mai LV, et al. The first epidemiology of urolithiasis in Northern Vietnam: Urinary stone composition, age, gender, season, and clinical features study. Urologia. 2024;91(1):42-8.
-
Evan AP. Physiopathology and etiology of stone formation in the kidney and the urinary tract. Pediatr Nephrol. 2010;25(5):831-41.
-
Brikowski TH, Lotan Y, Pearle MS. Climate-related increase in the prevalence of urolithiasis in the United States. Proc Natl Acad Sci U S A. 2008;105(28):9841-6.
-
Gambaro G, Croppi E, Coe F. et al. Metabolic diagnosis and medical prevention of calcium nephrolithiasis and its systemic manifestations: a consensus statement. J Nephrol. 2016;29(6):715-34.
-
Meng C, Peng L, Li J, Li Y, Li J, Wu J. Comparison between single-use flexible ureteroscope and reusable flexible ureteroscope for upper urinary calculi: a systematic review and meta-analysis. Front Surg. 2021;8(10):691170.
-
Dresner SL, Iremashvili V, Best SL, Hedican SP, Nakada SY. Influence of lower pole infundibulopelvic angle on success of retrograde flexible ureteroscopy and laser lithotripsy for the treatment of renal stones. J Endourol. 2020;34(6):655-60.
-
Karim SS, Hanna L, Geraghty R, Somani BK. Role of pelvicalyceal anatomy in the outcomes of retrograde intrarenal surgery (RIRS) for lower pole stones: outcomes with a systematic review of literature. Urolithiasis. 2020;48(3):263-70.
-
A Alenezi H, Denstedt JD. Flexible ureteroscopy: Technological advancements, current indications and outcomes in the treatment of urolithiasis. Asian J Urol. 2015;2(3):133-141.
-
Eisel M, Strittmatter F, Ströbl S. et al. Comparative investigation of reusable and single–use flexible endoscopes for urological interventions. Sci Rep. 2020;10(3):5701.
-
Ding J, Xu D, Cao Q, et al. Comparing the efficacy of a multimodular flexible ureteroscope with its conventional counterpart in the management of renal stones. urology. 2015;86(2):224-9.
-
Marchini GS, Torricelli FC, Batagello CA, et al. A comprehensive literature-based equation to compare cost-effectiveness of a flexible ureteroscopy program with single-use versus reusable devices. Int Braz J Urol. 2019;45(4):658-70.
-
Mazzucchi E, Marchini GS, Berto FCG, et al. Single-use flexible ureteroscopes: update and perspective in developing countries. A narrative review. Int Braz J Urol. 2022;48(3):456-67.
-
Pan WH, Yeh WT. How to define obesity? Evidence-based multiple action points for public awareness, screening, and treatment: an extension of Asian-Pacific recommendations. Asia Pac J Clin Nutr. 2008;17(3):370-4.
-
Schuster TG, Hollenbeck BK, Faerber GJ, Wolf JS. Ureteroscopic treatment of lower pole calculi: comparison of lithotripsy in situ and after displacement. J Urol. 2002;168(1):43-5.
-
Schoenthaler M, Wilhelm K, Katzenwadel A, et al. Retrograde intrarenal surgery in treatment of nephrolithiasis: is a 100% stone-free rate achievable? J Endourol. 2012; 26(5):489-93.
-
Mai VQ, Sun S, Minh HV, et al. An EQ-5D-5L Value Set for Vietnam. Qual Life Res. 2020;29(7):1923-33.
-
Salvadó JA, Olivares R, Cabello JM, et al. Retrograde intrarenal surgery using the single - use flexible ureteroscope Uscope 3022 (Pusen™): evaluation of clinical results. Cent European J Urol. 2018;71(2):202-7.
-
Jing Q, Liu F, Yuan X, Zhang X, Cao X. Clinical comparative study of single-use and reusable digital flexible ureteroscopy for the treatment of lower pole stones: a retrospective case-controlled study. BMC Urol. 2024;24(7):149.
-
He Q, Wei X, Wu E, Luo R, Yu L, Liang W. Comparison of percutaneous nephrolithotomy and flexible ureterorenoscopy in the treatment of single upper ureteral calculi measuring 1 to 2 centimeters: a retrospective study. BMC Urol. 2024;24(1):23.
-
Gao H, Zhang H, Wang Y, et al. Treatment of complex renal calculi by digital flexible ureterorenoscopy combined with single-tract super-mini percutaneous nephrolithotomy in prone position: a retrospective cohort study. Med Sci Monit. 2019;25(8):5878-85.
-
El-Nahas AR, Ibrahim HM, Youssef RF, Sheir KZ. Flexible ureterorenoscopy versus extracorporeal shock wave lithotripsy for treatment of lower pole stones of 10-20 mm. BJU Int. 2012;110(6):898-902.
-
Hao X, Li C, Dun W, Xia Q. Effect of flexible ureteroscopic lithotripsy on surgical outcomes, renal function and quality of life of patients with 2-3 cm renal calculi. Arch Esp Urol. 2023;76(3):189-95.
Figures
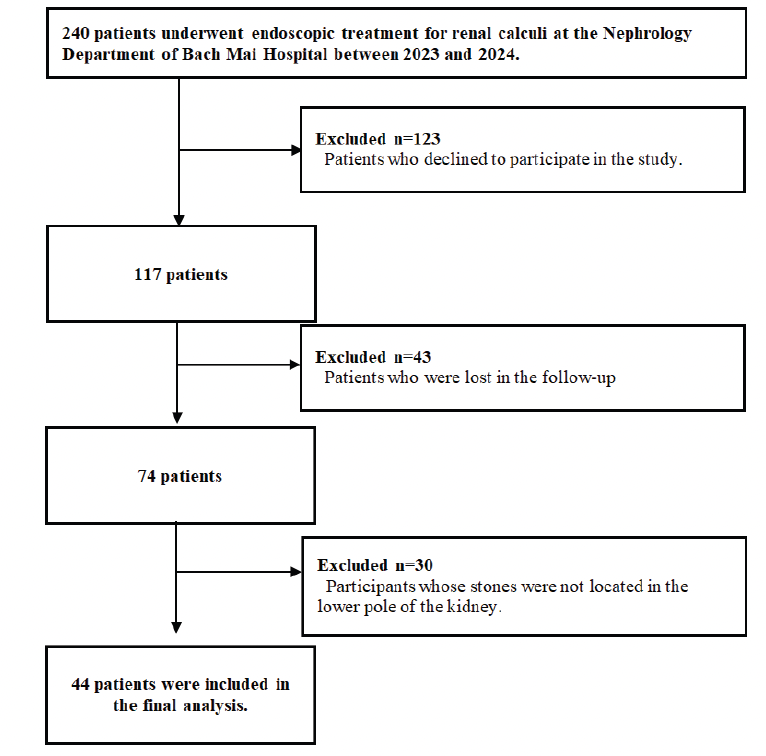
Figure 1. The flowchart of participants
Tables
Table 1. Characteristic of participants
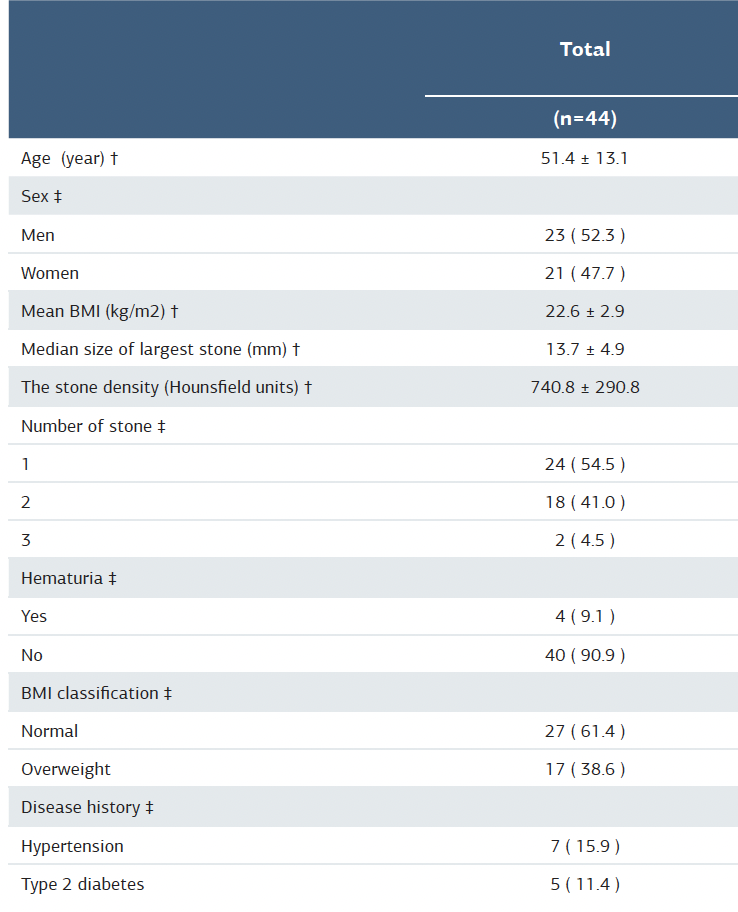
† Mean ± Standard deviation ‡ Number (%)
Table 2. Surgical and follow-up outcomes
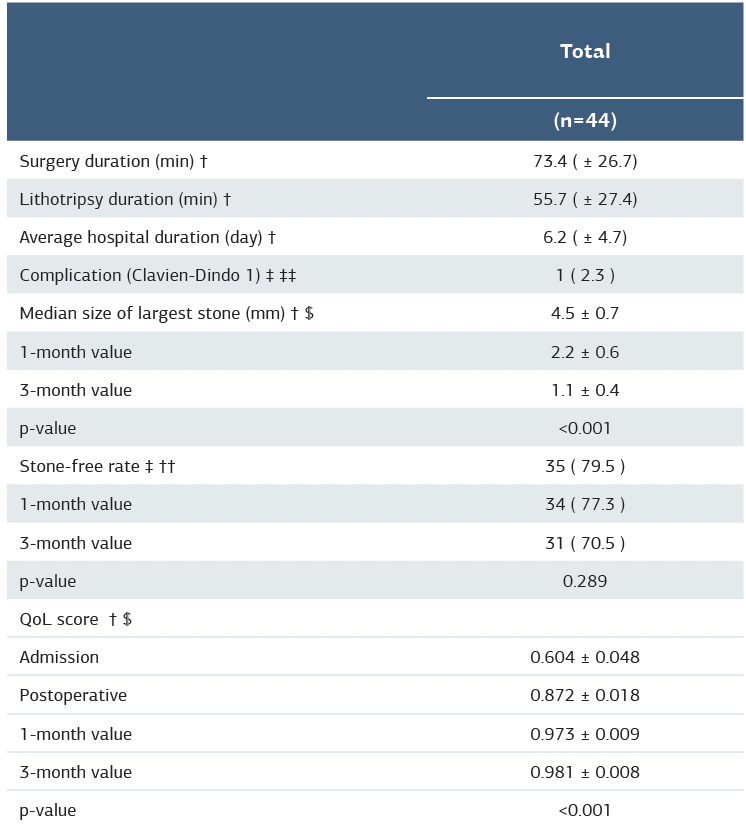
† Mean ± Standard deviation ‡ Number (%) $ Repeated measurement was used to compared mean and calculated p-value †† Mac-nemar test was used to compared proportions and calculated p-value
Additional Information
Publisher’s Note
Bayrakol MP remains neutral with regard to jurisdictional and institutional claims.
Rights and Permissions
About This Article
How to Cite This Article
Nguyen Huu Thanh, Nguyen Minh Tuan, Hoang Long, Dinh Anh Duc, Dong Ngoc Minh, Ngo Xuan Cuong, Nguyen Truong Giang, Tran Quoc Khanh, Nguyen Tuan Anh, Nguyen Thanh Vinh. Clinical efficacy of digital flexible ureteroscopy for renal stone management and postoperative quality of life for the treatment of lower pole stones: A single-center, non-randomized study. Ann Clin Anal Med 2025;16(10):736-740

