Sexually transmitted infection knowledge and misconceptions among university students in Türkiye
STI knowledge gaps among university students
Authors
Abstract
Aim Sexually transmitted infections (STIs) remain a major public health concern worldwide, particularly among young adults who often have incomplete or inaccurate knowledge regarding transmission, prevention, and clinical outcomes. In Türkiye, the lack of a structured national sexual health education program may contribute to persistent knowledge gaps among university students. This study aimed to assess awareness and knowledge of STIs among university students and to identify prevalent misconceptions.
Methods A cross-sectional online survey was conducted between May and December 2024 among undergraduate students in Türkiye. A structured 32-item questionnaire assessed sociodemographic characteristics, awareness of STIs, transmission routes, misconceptions, preventive behaviors, knowledge of the human immunodeficiency virus (HIV) “Undetectable = Untransmittable (U = U)” concept, and HPV-related knowledge. Descriptive statistics were used to summarize responses, and group comparisons were performed using appropriate statistical tests, with p < 0.05 considered significant.
Results A total of 424 students participated (mean age: 20.06 ± 1.98 years; 55.2% women). Most respondents (74.8%) had never received formal STI education, although 76.2% expressed a desire for training. Awareness was high for HIV (96.5%) and HPV (87.3%), but considerably lower for other STIs such as Trichomonas vaginalis (31.8%). Misconceptions were common; 26.4% believed HIV could be transmitted through swimming pools. Awareness of the U = U concept was very limited (7.5%), and only 11.8% reported receiving HPV vaccination.
Conclusion University students in Türkiye demonstrate important gaps and misconceptions regarding STIs, particularly in relation to transmission routes, HPV vaccination, and contemporary HIV concepts. These findings highlight the need for structured, evidence-based sexual health education programs targeting young adults in university settings.
Keywords
Introduction
Sexually transmitted infections (STIs) encompass a wide range of bacterial, viral, and parasitic infections transmitted primarily through sexual contact.1 According to the World Health Organization, more than one million curable STIs occur every day among individuals aged 15-49 years, a substantial proportion of which are asymptomatic and therefore remain undiagnosed.2 The silent nature of many STIs contributes to significant global morbidity, including pelvic inflammatory disease, infertility, adverse pregnancy outcomes, and increased susceptibility to human immunodeficiency virus (HIV) acquisition.1,2 Moreover, untreated or recurrent infections place a considerable economic burden on healthcare systems due to ongoing diagnostic, therapeutic, and follow-up requirements.
Despite the availability of reliable and sensitive diagnostic tests, many individuals delay seeking medical care because of stigma, embarrassment, cultural norms, or fear of discrimination.3,4 For these reasons, prevention strategies centered on education, awareness, and early counseling remain essential in reducing transmission. Young adults, particularly university students, constitute a key population in this context. This stage of life often coincides with the initiation of sexual activity, while knowledge about STIs, preventive measures, and asymptomatic transmission may remain incomplete. Studies conducted in various countries consistently show that young people frequently harbor misconceptions regarding transmission routes, symptoms, and prevention, despite reporting general awareness of STIs.5,6,7,8,9
In our country, the lack of a structured, evidence-based national sexual health education curriculum further amplifies these challenges. Cultural and religious sensitivities often limit open discussion about sexual health within families, leaving adolescents with limited or unreliable information prior to university.5 Local studies have shown that Turkish university students frequently exhibit insufficient knowledge regarding STI risks and prevention, and that self-perceived knowledge does not consistently align with objective assessments.5,6 Moreover, awareness of contemporary topics—such as the cancer-related risks of human papillomavirus (HPV) and the importance of vaccination—remains suboptimal. Similarly, knowledge of HIV-related advances, including the “Undetectable = Untransmittable (U = U)” principle, is limited among young adults.7,10,11,12,13
The increasing role of digital media in shaping health information underscores the need to understand modern patterns of STI knowledge among university students. International research highlights persistent gaps in awareness of HPV vaccination, HIV prevention strategies, and the possibility of asymptomatic STI transmission, despite the widespread use of online information sources.7,8,9,10,11
Materials and Methods
Study Design and SettingThis cross-sectional study was conducted to assess university students’ awareness and knowledge of STIs in Türkiye. Data was collected using an online self-administered questionnaire distributed between May and December 2024. The survey targeted undergraduate students enrolled in various universities across the country, representing different regions and academic disciplines.
Study Population and Sample SizeThe study population consisted of undergraduate students aged 18–30 years. The minimum required sample size was calculated using classical prevalence-based formulas, assuming a 50% expected level of STI knowledge (the most conservative estimate), a 95% confidence interval, and a 5% margin of error. Under these assumptions, the minimum sample size was determined to be 384 participants.
To account for potential non-response or incomplete submissions—commonly ranging from 5% to 15% in online surveys—a 10% oversampling strategy was applied. A total of 424 students completed the questionnaire and were included in the final analysis.
Data Collection ToolData was gathered using a structured questionnaire developed within the scope of the Faculty of Medicine Term I Special Study Module (SSM) group. As part of the SSM process, Term I medical students reviewed evidence-based literature on STIs, participated in peer-learning activities, and collaboratively generated an initial pool of survey items.
This item pool was subsequently reviewed and refined by a multidisciplinary expert panel, including an infectious diseases specialist, a medical education specialist, a family medicine specialist, and an anesthesiology and reanimation specialist. This ensured both content validity and clarity of the questionnaire.
The final version of the questionnaire consisted of 32 items (Supplementary Table 1).
• Sociodemographic characteristics (7 items): age, gender, university, faculty, academic year, and region of residence.
• Awareness and knowledge items (25 items):
o Sources of STI information,
o Condom use and preventive behaviors,
o Transmission routes and common misconceptions,
o Symptom recognition,
o HIV-related concepts (including U = U),
o Awareness of HPV and HPV vaccination.
Items were informed by CDC guidelines and contemporary epidemiological evidence,1 as well as national and international literature documenting knowledge gaps among young adults.5-12 Including student participation in item generation is aligned with evidence supporting peer-based approaches to sexual health education.13,14
Data Collection ProcedureThe survey was administered online using a secure web-based form. Participation was voluntary and anonymous. Students were informed that the questionnaire aimed to assess their general knowledge about STIs and did not require prior medical training.
Ethical ApprovalThis study was approved by the Ethics Committee of Buca Seyfi Demirsoy Training and Research Hospital (Date: 2024-04-24, No: 271).
Statistical AnalysisData was analyzed using IBM SPSS Statistics version 25. Descriptive statistics (frequency, percentage, mean, and standard deviation) were used to summarize participant characteristics and response patterns.
Normality of continuous variables (e.g., age) was assessed using the Shapiro–Wilk test. Since age followed a normal distribution, group comparisons were performed using independent samples t-tests and one-way ANOVA where appropriate.
Categorical variables and Likert-scale responses were compared using Pearson’s chi-square test. Statistical significance was set at p < 0.05.
Reporting GuidelinesThis study is reported in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines.
Results
A total of 424 university students participated in the study. The mean age of the participants was 20.06 ± 1.98 years (range: 18–30). Of all respondents, 55.2% were women and 44.1% were men. More than half of the sample consisted of students from health-related faculties (including medical/dentistry and other health sciences), and 53.5% were first-year students (Table 1). The detailed distributions by region of origin, current study region, and university are provided in Supplementary Table 2.
Awareness and Experience Related to STI EducationMost participants (74.8%) reported that they had never received any formal education on STIs. Nevertheless, more than three-quarters of the students (76.2%) expressed a willingness to receive STI-related training. Among those who had received education (25.2%), the most common settings were high school (7.1%) and university courses (12%).
Most respondents indicated that STI education should be provided during high school (68.9%), while smaller proportions preferred middle school (13.7%) or university-level instruction (16.3%). The detailed distribution of previous STI education sources and training preferences is presented in Supplementary Table S3.
Sources of Information and Recognition of STIs
Social media and internet platforms were the most frequently reported sources of STI information (83.3%), followed by peers (57.3%) and school-based resources (37.3%). In contrast, books (1.2%) and non-governmental organizations (9.2%) were rarely cited.
Participants most recognized HIV (96.5%), HPV (87.3%), and gonorrhea (73.4%) as STIs. Awareness of other STIs, such as Trichomonas vaginalis (31.8%) and chancroid (17.0%), was considerably lower.
Knowledge of STI Transmission and MisconceptionsNearly all participants identified unprotected sexual intercourse (97.9%) and needle-sharing (70.3–78.1%) as risk factors for HIV transmission. Whereas misconceptions about non-transmissible routes such as swimming pools (26.4%), insect bites (25.0%), and public transportation (3.8%) persisted.
Among the participants, 31.6% agreed with the statement “I have sufficient knowledge about STIs,” while 7.3% strongly agreed. However, 40.6% reported being undecided on this matter.
More than half (53.3%) agreed that STIs may present without symptoms, and 24.5% strongly agreed.
A substantial proportion (34.7%) incorrectly believed that STIs could be transmitted via door handles, toilet seats, or faucets (Table 2).
Regarding statement-based specific knowledge, most participants demonstrated an accurate understanding of several key issues. A total of 67.3% correctly rejected the idea that HIV can be transmitted through kissing, reflecting an appropriate grasp of established transmission routes. However, uncertainty remained in other areas, as 58.0% of students were unsure whether hepatitis C has an effective treatment. Preventive practices were distinctly acknowledged, with 61.1% of respondents agreeing or strongly agreeing that condom use mitigates STI transmission risk. In contrast, misconceptions persisted regarding contraception, with 75.2% correctly disagreeing that birth control pills offer protection against STIs.
Attitudes, Testing Behaviors, and Awareness of U = UMost respondents (92.9%) indicated they would inform their partner if they had an STI, and 98.6% reported that they had never received treatment for an STI. Only 10.4% had been tested for an STI. Awareness of the “Undetectable = Untransmittable (U = U)” concept was low, 92.5% stated that they had never heard of U = U, and only 4.7% provided a correct explanation (Table 3).
HPV Knowledge and VaccinationAwareness of HPV-related risks was moderate, 70.0% knew that HPV is a sexually transmitted virus that can cause cancer, and 20.3% reported no knowledge on the subject.
HPV vaccination rates were low, with only 11.8% of participants reporting prior vaccination (Table 3).
Discussion
This study revealed substantial gaps in university students’ awareness and knowledge of STIs in Türkiye, despite a generally positive attitude toward receiving STI education. The majority of participants reported never having received formal STI training, and only a minority felt that they possessed sufficient knowledge. These findings are consistent with national and international literature showing that young adults frequently exhibit incomplete or inconsistent understanding of STI transmission routes, symptoms, prevention strategies, and long-term consequences.5,6,7,8,9
A prominent result of this study was that although students widely recognized well-known infections such as HIV and HPV, knowledge about other STIs—such as Trichomonas vaginalis infection or chancroid was markedly limited. This pattern parallels findings from studies conducted in Malaysia, Ethiopia, Italy, and other settings, where awareness is strongly skewed toward HIV while other STIs remain poorly understood.7,8,9 Such disparities may reflect the unequal visibility of different infections in public health campaigns and digital media and highlight the need for more comprehensive sexual health education that covers the full spectrum of STIs.
Misconceptions about transmission routes were also common in our sample. While the majority of students accurately recognised unprotected sexual intercourse and needle sharing as risk factors, a significant number held the misconception that HIV could be transmitted via casual contact, including swimming pools or insect bites. Similar misconceptions have been reported internationally, suggesting that misunderstanding of nonsexual transmission remains a pervasive barrier to effective STI prevention.7 These inaccuracies not only misdirect personal risk assessment but may also contribute to persistent stigma toward individuals living with HIV or other STIs.
Participants showed relatively better understanding of asymptomatic infection; more than half recognized that STIs may not always present symptoms. This finding is encouraging and aligns with increasing public dissemination of information on asymptomatic carriers—particularly in WHO and CDC materials.1,2 However, the low proportion of students who had ever been tested for an STI indicates that knowledge of asymptomatic infection does not necessarily translate into preventive health behaviors. This discrepancy between knowledge and action has been emphasized in previous studies across diverse cultural contexts.6,7,8,9
A particularly striking finding was the extremely low awareness of the “Undetectable = Untransmittable (U = U)” principle. More than 90% of participants had never heard of the concept, and only a small fraction could explain it correctly. Recent literature underscores the importance of U = U in reducing stigma, improving treatment uptake, and supporting public health messaging.12,13 The lack of awareness in our sample suggests that major advances in HIV science have not yet been adequately reflected in the knowledge of young adults in Türkiye. Incorporating U = U into sexual health curricula may therefore improve both scientific understanding and social attitudes toward people living with HIV.
HPV-related knowledge showed a similar pattern of partial understanding. Although the majority correctly identified HPV as an STI associated with cancer development, vaccination rates were notably low. This is consistent with studies from Germany and Poland, which reported moderate awareness but low vaccination uptake among adolescents and young adults.10,11 Barriers may include lack of access, cost, inconsistent public information, or insufficient integration into school-based health programs. Given the rising global emphasis on HPV vaccination as a cancer prevention strategy, strengthening educational outreach in this area remains a critical need.
The findings of this study also reinforce the importance of modern, technology-supported educational approaches. Students primarily relied on social media and internet platforms for STI information, echoing trends observed in studies where digital interventions such as peer-created short-form videos or podcast-based STI curricula—successfully improved knowledge and maintained long-term learning effects.14,15 These methods may be particularly well suited for university populations who already engage regularly with digital content.
Overall, when interpreted alongside existing national and international studies, our results demonstrate several consistent themes: university students possess fragmented STI knowledge; misconceptions remain widespread; awareness does not always translate into preventive behavior; and education on HPV vaccination and U = U is particularly lacking. At the same time, students express high interest in receiving STI education, offering an important opportunity for implementing modern, structured, evidence-based sexual health programs.
In line with these findings, our research group also implemented a peer-led sexual health education initiative within the Faculty of Medicine Special Study Module (SSM) in the following academic year. This program involved structured STI-focused training delivered by medical students to university students, accompanied by pre- and post-education assessments to evaluate learning outcomes. Preliminary observations indicated substantial improvements in post-training knowledge scores, supporting the effectiveness of peer-based educational strategies for addressing misconceptions and enhancing STI awareness among young adults. Integrating such sustainable, student-centered models into university curricula may serve as a practical and impactful approach to reducing the knowledge gaps identified in this study and improving sexual health literacy more broadly in Türkiye.
Limitations
Regarding the interpretation of the findings, it is important to take into account the fact that this study contains a number of limitations. First, the cross-sectional methodology prevents causal conclusions between sociodemographic characteristics and STI knowledge levels. Secondly, data were gathered using a self-administered online questionnaire, which may be susceptible to recollection bias and social desirability bias. Third, despite the participation of students from various institutions and areas, the sample had a disproportionately large number of medical and health-related students, thereby constraining the generalisability of the findings to the broader university community. Finally, STI knowledge was assessed based on self-reported responses rather than objective testing, which may not fully reflect actual knowledge or behavior. Notwithstanding these constraints, the study offers significant and current insights regarding STI knowledge and misconceptions among university students in Türkiye.
Conclusion
This study demonstrated that university students in Türkiye have fragmented and often insufficient knowledge of sexually transmitted infections, with notable misconceptions regarding transmission routes, preventive practices, and the clinical course of STIs. Awareness of HPV-related risks and the U = U principle was particularly low, despite the public health importance of these topics. At the same time, students expressed a strong willingness to receive STI education, indicating a significant unmet need.
The findings highlight the critical importance of integrating structured, evidence-based sexual health education into university settings and, ideally, initiating such education earlier in adolescence. Peer-led learning models, such as the educational intervention later implemented within our Special Study Module (SSM), show promise as an effective and sustainable strategy to improve STI knowledge among young adults. Expanding and formalizing such student-centered approaches may contribute meaningfully to enhancing sexual health literacy and reducing STI-related risks across university populations in Türkiye.
Declarations
Ethics Declarations
This study was approved by the Ethics Committee of Buca Seyfi Demirsoy Training and Research Hospital (Date: 2024-04-24, No: 271).
Animal and Human Rights Statement
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Participation was voluntary and anonymous. Electronic informed consent was obtained from all participants prior to completing the online questionnaire. Participants were informed about the study purpose and their right to withdraw at any time.
Data Availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Conflict of Interest
The authors declare that there is no conflict of interest.
Funding
None.
Author Contributions (CRediT Taxonomy)
Conceptualization: N.S.
Methodology: N.S., A.B.
Formal Analysis: N.S., A.B.
Investigation: N.S.
Data Curation: N.S.
Writing – Original Draft Preparation: N.S.
Writing – Review & Editing: A.B., P.A.
Supervision: A.B., P.A.
Scientific Responsibility Statement
The authors declare that they are responsible for the scientific content of this manuscript, including study design, data collection, analysis and interpretation of data, drafting and revising the manuscript, and approval of the final version.
Abbreviations
STI: Sexually transmitted infection
SSM: Special Study Module
WHO: World Health Organization
HIV: Human Immunodeficiency Virus
U = U: Undetectable = Untransmittable
HPV: Human Papilloma Virus
CDC: Centers for Disease Control and Prevention
References
-
Workowski KA, Bachmann LH. Sexually transmitted infections treatment guidelines, 2021. Clin Infect Dis. 2022;74(Suppl 2):S89-S94. doi:10.1093/cid/ciab1055
-
World Health Organization. Sexually transmitted infections (STIs). World Health Organization. Updated 2024. Accessed January 12, 2025. https://www.who.int/news-room/fact-sheets/detail/sexually-transmitted-infections-(stis)
-
Alshemeili A, Alhammadi A, Alhammadi A, et al. Sexually transmitted diseases knowledge assessment and associated factors among university students in the United Arab Emirates: a cross-sectional study. Front Public Health. 2023;11:1284288. doi:10.3389/fpubh.2023.1284288
-
Aseeri IA, AlOtaibi MN, Alzahrani WJ, et al. Public awareness about sexually transmitted diseases in Taif, Saudi Arabia. Cureus. 2023;15(7):e42302. doi:10.7759/cureus.42302
-
Yıldırım F, Erbil N. Knowledge level about sexually transmitted diseases among university students in Türkiye: a systematic review. Androl Bul. 2021;23:179-186.
-
Karakose A, Aydın S. Evaluation of young men’s level of knowledge about sexually transmitted diseases. New J Urol. 2011;6(1):31-37
-
Folasayo AT, Oluwasegun AJ, Samsudin S, et al. Assessing the knowledge level, attitudes, risky behaviors and preventive practices on sexually transmitted diseases among university students as future healthcare providers in the central zone of Malaysia: a cross-sectional study. Int J Environ Res Public Health. 2017;14(2):159. doi:10.3390/ijerph14020159
-
Cegolon L, Bortolotto M, Bellizzi S, et al. A survey on knowledge, prevention, and occurrence of sexually transmitted infections among freshmen from four Italian universities. Int J Environ Res Public Health. 2022;19(2):897. doi:10.3390/ijerph19020897
-
Nigussie T, Yosef T. Knowledge of sexually transmitted infections and its associated factors among polytechnic college students in Southwest Ethiopia. Pan Afr Med J. 2020;37:68. doi:10.11604/pamj.2020.37.68.22718
-
Rummel M, Clanner-Engelshofen BM, Nellessen T, et al. Evaluation of the knowledge of students concerning sexually transmitted infections in Bavaria/Germany (a cross-sectional study). J Dtsch Dermatol Ges. 2022;20(2):169-176. doi:10.1111/ddg.14653
-
Sypień P, Zielonka TM. Evaluation of Polish adolescents’ knowledge about human papillomavirus and vaccines. J Adolesc Young Adult Oncol. 2023;12(3):376-382. doi:10.1089/jayao.2022.0054
-
Wells N, Richman B, Grace D, et al. 2023 Undetectable = Untransmittable global policy roundtable report: a multistakeholder perspective on Undetectable = Untransmittable research and policy priorities. Sex Health. 2024;21:SH24017. doi:10.1071/SH24017
-
Georgiadis N, Katsimpris A, Halkitis PN, et al. Undetectable = Untransmittable: a cross-population systematic review and meta-analysis on awareness and acceptance. Pathogens. 2025;14(7):673. doi:10.3390/pathogens14070673
-
Dolu İ, Bozkurt FD, Bulut E, et al. Do peer-based short-form educational videos created by nursing students improve youths’ knowledge of sexually transmitted diseases? A quasi-experimental study. Int J Nurs Pract. 2024;30(3):e13221. doi:10.1111/ijn.13221
-
Ramchandani MS, Bauer KM, Freimund JS, et al. The National Sexually Transmitted Disease Curriculum podcast as a method to increase sexually transmitted infection education for health care professionals. Sex Transm Dis. 2024;51(7):452-455. doi:10.1097/OLQ.0000000000001970
Tables
Table 1. Summary of sociodemographic characteristics of the participants (n = 424)
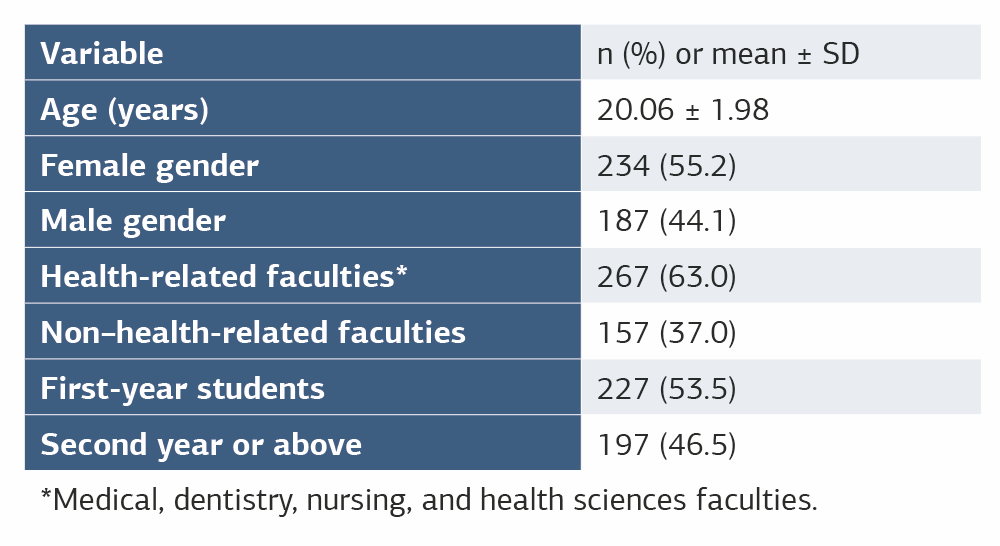
*Medical, dentistry, nursing, and health sciences faculties.
Table 2. Participants’ knowledge regarding STI-related statements
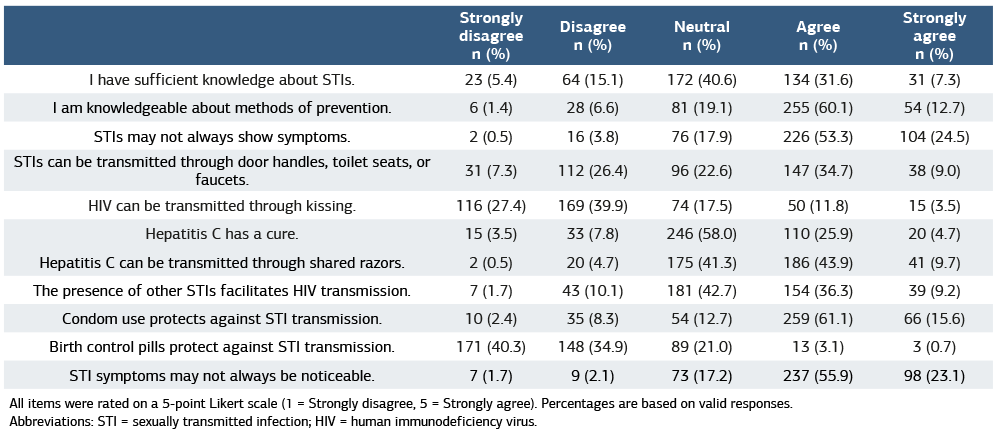
All items were rated on a 5-point Likert scale (1 = Strongly disagree, 5 = Strongly agree). Percentages are based on valid responses. Abbreviations: STI = sexually transmitted infection; HIV = human immunodeficiency virus.
Table 3. Participants’ attitudes, testing behaviors, and HPV vaccination status
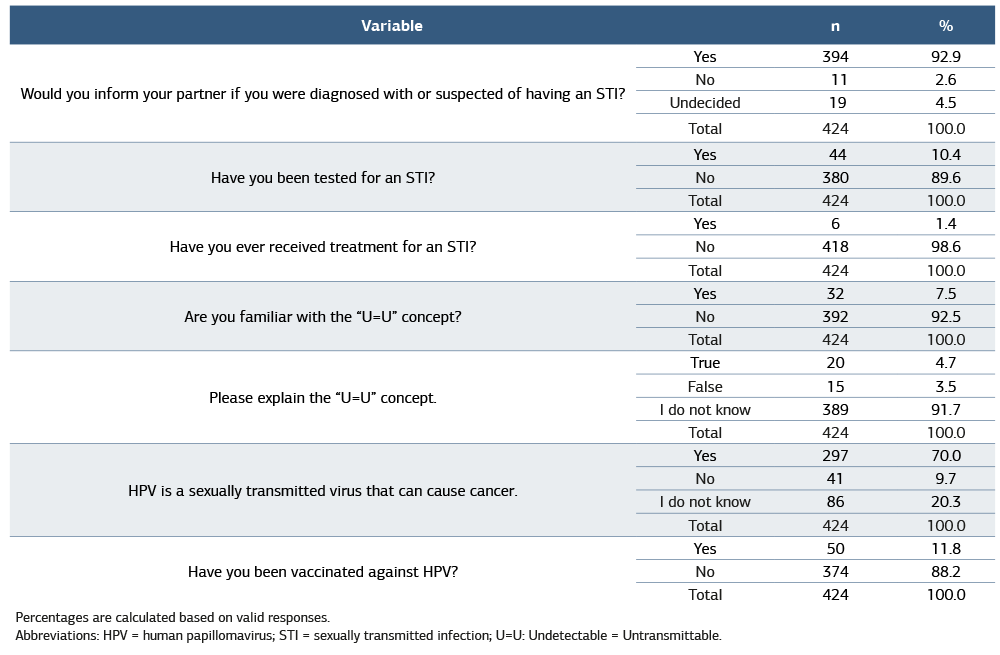
Percentages are calculated based on valid responses. Abbreviations: HPV = human papillomavirus; STI = sexually transmitted infection; U=U: Undetectable = Untransmittable.
Additional Information
Publisher’s Note
Bayrakol MP remains neutral with regard to jurisdictional and institutional claims.
Rights and Permissions
About This Article
How to Cite This Article
Nurbanu Sezak, Aysel Baser, Pınar Ayvat. Sexually transmitted infection knowledge and misconceptions among university students in Türkiye. Ann Clin Anal Med 2026;17(3):232-237
- Received:
- December 23, 2025
- Accepted:
- February 19, 2026
- Printed:
- March 1, 2026

