Reversing the traditional sequence in anatomy education: a practice-first experiential learning study
Practice-first anatomy
Authors
Abstract
Aim To evaluate the feasibility of implementing a practice-first Kolb experiential learning sequence in anatomy education and to examine its short-term effects on students’ educational model preferences, study habits, and self-efficacy.
Methods This single-group before-and-after interventional study was conducted during the 2023–2024 spring semester. The intervention included laboratory-based exposure (donated body dissection, prosected specimens, 3D-printed models), reflective discussion, interactive lectures, and an open laboratory session. Pre- and post-intervention surveys assessed demographics, study habits, educational model preference, and self-efficacy. Quantitative data were analyzed using IBM SPSS v23, and qualitative responses were evaluated through thematic analysis.
Results Of 166 students invited, 119 completed the pre-intervention survey (71.7%), and 66 completed the matched post-intervention survey (55.5%). Preference for the practice-first model increased from 21% to 36% (McNemar p<0.001). Switching to the practice-first model was associated with higher weekly study hours (p = 0.016) and preparedness (OR = 9.3; 95% CI 2.0–43.2; p = 0.013). No significant change was observed in self-efficacy (p = 0.219).
Conclusion A practice-first Kolb-aligned sequence is feasible and can significantly shift educational preferences in the short term. Behavioral factors appear critical, whereas longer exposure may be required to influence self-efficacy.
Keywords
Introduction
Anatomy is a core component of medical education and is traditionally taught through lectures supported by donated body dissection, prosections, anatomical models, and radiological imaging, which transform abstract knowledge into concrete understanding and enhance retention.1,2
Contemporary medical students, shaped by digital environments, tend to benefit from interactive and experiential learning approaches.3 Student-centered models such as the flipped classroom and problem-based learning (PBL) have been associated with improved student satisfaction and academic performance4,5 and reflect the principles of Kolb’s Experiential Learning Cycle (concrete experience → reflective observation → abstract conceptualization → active experimentation).6 In this framework, learning begins with concrete experience, which shapes subsequent reflection and conceptual understanding.7,8 Kolb-based approaches in health sciences education have been consistently linked to improved learning outcomes and strengthened reflective practice.7,9 Despite these advantages, anatomy teaching continues to rely predominantly on a “theory-first, practice-second” sequence, a structure that remains debated in light of experiential learning principles.8,9
Against this theoretical background, initiating anatomy education with laboratory exposure represents a coherent extension of experiential learning principles. A practice-first sequence enables learners to encounter anatomical structures through donated body dissection, prosections, or 3D-printed models before formal instruction, potentially fostering active engagement and facilitating the integration of theoretical knowledge with clinical application.10,11,12
From a complementary cognitive perspective, Cognitive Load Theory (CLT) provides a mechanistic explanation for this sequencing. By positioning concrete experience at the beginning of the learning process, abstract concepts may be anchored to emerging schemas, which can reduce extraneous cognitive load and support germane processing within working-memory limits.13,14,15,16
Although preliminary evidence suggests that prioritizing concrete experiences may enhance understanding and promote clinical skill development,17 the cognitive and pedagogical implications of reversing the traditional “theory-first” sequence in routine anatomy education remain insufficiently explored.
Accordingly, the present study evaluates the feasibility of implementing a practice-first, Kolb-aligned instructional sequence in anatomy education. In addition, students’ preferences regarding instructional sequencing are examined before and after exposure to both traditional and reversed orders. The findings are expected to inform future restructuring of anatomy curricula.
Materials and Methods
Study Design and SettingThis study was conducted during the spring semester of the 2023–2024 academic year as a single-group before-and-after interventional study using survey-based data collection. Predefined study quality benchmarks were: enrollment ≥ 70%, completion ≥ 50%, and Cronbach’s α ≥ 0.70 for multi-item scales. Sessions that included donated body dissections, prosected specimens, and 3D-printed models were designated as practical sessions, whereas slide supported amphitheater lectures were designated as didactic sessions.
Sessions that included donated body dissections, prosected specimens, and 3D-printed models were designated as practical classes, while lecture-hall sessions supported by slides were designated as theoretical classes. A total of 119 students completed the pre-intervention survey, and 66 students completed the matched post-intervention survey. Participation was voluntary and anonymous, with electronic informed consent obtained. Records with inconsistent codes or missing consent were excluded. Figure 1 presents the schematic comparison of the traditional (didactic-first) and experimental (practice-first) sequences.
Educational Intervention (practice-first Kolb sequence)The intervention lasted for two weeks and was structured according to Kolb’s Experiential Learning Cycle6 (Figure 2):
● Concrete experience: two × 50-minute practical sessions involving donated body dissection, prosected specimens, 3D-printed models, and atlases; approximately 10–15 students per table, each supervised by an MD-PhD instructor with at least three years of experience.
● Reflective observation: a 30-minute small-group discussion followed by a 250-word reflective writing assignment.
● Abstract conceptualization: two × 50-minute interactive didactic sessions in the same week, supported by slides, concept maps, and clinical vignettes.
● Active experimentation: a 100-minute Open Lab, allowing independent repetition with prosected specimens and 3D models.
No additional examination or grading was performed.
Measures and Data CollectionThe data were collected in four domains before the intervention. These were demographic data, Study Habits through a four-point Likert scale (Always–Often–Rarely–Never), and academic indicators such as the score obtained in the final block examination conducted at the end of the 2023–2024 fall semester and weekly study hours. In addition, students were asked to indicate their baseline educational model preference, choosing between the didactic-first and practice-first sequences.
After implementation of the practice-first Kolb sequence (intervention), the data on each student’s final preference and rationale, a self-efficacy item in which participants rated the statement “I am ready to apply this regional anatomy” for both sequences using a five-point Likert scale. Finally, two open-ended questions invited students to describe the strengths and weaknesses of each of the didactic-first and practice sequences and to elaborate on how these approaches influenced their learning process. The full questionnaire texts, along with their English translations, are provided in Supplementary Table 1.
Questionnaire Design and ValidityThe questionnaire items were developed with reference to Kolb’s literature.18,19 Content validity was evaluated independently by three senior anatomists. Internal consistency for the Study Habits scale (five items) was acceptable, with a Cronbach’s α of 0.724.20
Data Collection and PrivacyThe questionnaires were administered via Google Forms, and links were distributed through the class representative through a WhatsApp group. Participation required electronic informed consent. Responses before and after intervention were matched using a unique code known only to the participant; records with inconsistent codes or missing consent were excluded. All data were stored and reported in accordance with confidentiality principles.
Ethical ApprovalThis study was approved by the Non-Interventional Clinical Research Ethics Committee of Medipol University (Date: 2024-05-22, No: 513). It involved voluntary participation of medical students and did not include patient data or identifiable information.
Statistical AnalysisAll analyses were performed using IBM SPSS Statistics v23, with statistical significance set at α = 0.05. Continuous variables were expressed as mean ± standard deviation (SD) or as median (minimum–maximum), while categorical variables were reported as frequency (n) and percentage (%). The normality of distributions was assessed with the Shapiro–Wilk test. Changes in educational-model preference across matched pairs were examined with the McNemar test, and changes in self-efficacy scores were analyzed with the Wilcoxon Signed-Rank test. Comparisons of continuous variables between two groups were carried out using either the Student’s t-test or the Mann–Whitney U test, depending on distributional assumptions. Associations between categorical variables were examined with the Pearson Chi-Square test or, when appropriate, the Fisher’s exact test. In addition, the relationship between preparedness and preference change was quantified by calculating the Odds Ratio (OR) with 95% Confidence Intervals (CI). Between-group comparisons (matched post-intervention survey completers vs pre-intervention survey–only participants) used appropriate parametric or non-parametric tests for continuous variables and Pearson’s Chi-Square or Fisher’s exact test for categorical variables.
Qualitative data from open-ended responses were analyzed using Braun and Clarke’s six-phase thematic analysis approach.21 Coding was conducted independently by two researchers, after which consensus was reached to finalize the themes. The results were illustrated with anonymized quotations from student responses.
Reporting GuidelinesThis study was conducted and reported in accordance with STROBE.
Results
Feasibility & Participant FlowIn this before-and-after interventional study, all 166 first-year medical students enrolled in the anatomy course were invited to participate. A total of 119 students completed the pre-intervention survey, yielding a 71.7% enrollment rate, which exceeded the predefined threshold of ≥ 70%. Among these students, 66 completed the matched post-intervention survey, corresponding to a 55.5% completion rate, also surpassing the feasibility criterion of ≥ 50%.
Baseline Demographics & Study HabitsA total of 119 students participated in the pre-intervention survey phase. Of these, 70.6% were male (n = 84) and 29.4% were female (n = 35). In the matched post-intervention survey phase, the sample decreased to 66 students, with 60.6% male (n = 40) and 39.4% female (n = 26). The mean age of male students was 19.13 ± 0.98 years at pre-intervention and 19.02 ± 0.96 years at post-intervention. For female students, the mean ages were 18.94 ± 1.06 years and 18.77 ± 0.82 years, respectively.
Detailed demographic characteristics are summarized in Table 1, which presents age (Mean ± SD) and gender distributions across both pre- and post-intervention survey phases.
Students reported that they studied an average of 9.75 ± 6.01 hours per week and scored 69.01 ± 12.51 points in the final block examination conducted at the end of the 2023–2024 fall semester. Preparation for practical courses (55.5%) was higher than for didactic courses (17.6%). Same day review habits were limited: 66.4% reported “never” or “rarely” revisiting content on the day it was taught. Participation in individual study sessions was also moderately distributed. These findings are presented in Supplementary Figures 1, panels A through D.
Educational-Model Preference and ChangeAccording to the data collected before the intervention, 79% of students (n = 94) preferred the traditional didactic-first sequence, while 21% (n = 25) favored the experimental practice-first sequence. The data collected from 66 participants after the intervention revealed that the proportion preferring the didactic-first sequence decreased to 64% (n = 42), whereas preference for the practice-first sequence increased to 36% (n = 24).
Longitudinal analysis of 66 students revealed that 26.8% (n = 15) shifted from didactic-first to practice-first, while only 1.5% (n = 1) shifted in the opposite direction. This change was statistically significant according to the McNemar test (p = 0.001). Details are presented in Table 2.
Predictors of Preference ChangeStudents who shifted to the experimental practice-first sequence reported studying an average of 13.33 ± 6.21 hours per week, compared with 8.98 ± 5.96 hours among those who did not change their preference (independent t-test, p = 0.016). Preparedness was also a significant predictor: the proportion of students who switched was 31.8% among those who came prepared for class, but only 4.5% among those who did not (Fisher’s exact test, p = 0.013). The strength of this association was quantified as OR = 9.3; 95% CI 2.0–43.2. No significant associations were observed with age, sex, or prior exam score (all p > 0.05). A summary of these findings is provided in Supplementary Table 2 and Supplementary Figure 2 and 3.
Self-Efficacy OutcomesThere was no significant difference in students' sense of efficacy after both models (p = 0.219; Supplementary Figure 4). This result shows that both models provide a similar level of learning competence.
Differences According to Survey ParticipationThere was no significant difference in study habits and exam success between the students who participated in the pre-intervention and post-intervention surveys together and those who participated only in the pre-intervention survey. However, the rate of practical class preparation differed significantly between the two groups (p = 0.009).
Feedback on the Experimental Education ModelThe open-ended responses of 36 students were analyzed thematically and grouped under three main themes:
● Contribution of visual and concrete experiences to theoretical understanding (71.4%): Students emphasized that donated body dissection and 3D models helped concretize structures, improved visualization, and supported retention.
● Transition from general knowledge to in-depth understanding (22.9%): The general knowledge provided by practical lessons helped students to grasp the theoretical details more easily. Repetition of complex topics in both practical and theoretical sessions reinforced understanding.
● Motivational contribution (5.7%): Practical sessions helped students better prepare for the course and increased their motivation and sense of responsibility for learning.
The opinions expressed under these three themes reveal that the experimental model positively affected students in conceptual but also in affective and behavioral dimensions (Supplementary Table 3).
Reasons for the Preference of the Education ModelIn the thematic analysis of 43 students who answered the open-ended question in the post-intervention survey, it was seen that those who preferred the traditional model (60.5%) emphasized the reasons for ‘concrete representation’ and ‘ease of preparation’ the most. Those who preferred the experimental model (39.5%) expressed reasons such as ‘concretization of abstract concepts’ and ‘adaptation to personal learning style’ more frequently. In both groups, ‘permanence of learning’ was the common emphasis (Supplementary Figure 5).
Discussion
This study demonstrates that a practice-first, Kolb-aligned sequence is feasible in anatomy education and can shift students’ instructional preferences in the short term. Increased weekly study time and preparedness were associated with this shift, and qualitative findings highlighted enhanced motivation and conceptual depth. No significant short-term change was observed in self-efficacy, suggesting that longer or repeated learning cycles may be required to influence this construct.
These findings are consistent with experiential learning applications in health professions education, which emphasize that meaningful practical engagement forms the basis for reflective observation and conceptual development.10,22 In anatomy education specifically, experiential and practice-oriented approaches have been shown to enhance student participation and perceived relevance.7,17 The present results extend this literature by suggesting that not only learning outcomes but also instructional sequencing preferences may shift when learners are first exposed to concrete anatomical experience.
From a cognitive perspective, initiating learning with concrete experience may help anchor abstract concepts to emerging schemas, thereby facilitating germane cognitive processing.13,14,15 Although cognitive load was not directly measured in this study, the observed behavioral shift may indirectly reflect this scaffolding effect.
Determinants of Preference ShiftTwo clear signals emerged as determinants of preference change: regular study and preparedness. This finding is consistent with previous studies demonstrating links between medical students’ study approach and time management and their learning outcomes.16 These results suggest that the benefits of the practice-first sequence depend not only on the pedagogical order but also on students’ active engagement in their own learning. Therefore, future implementations should consider integrating pre-class preparation (such as assigned readings, short videos, or pre-quizzes) as a standard component.
Self-EfficacyThe absence of a significant increase in self-efficacy may be explained by several factors. First, the measurement window was short. Second, the use of a single-item measure may have limited sensitivity, whereas multi-item, domain-specific scales are more robust.23,24 Third, improvements in self-efficacy typically require mastery experiences, which may emerge only after longer or repeated learning cycles and the inclusion of objective performance measures. Future studies should therefore employ multi-item self-efficacy scales alongside objective tests of knowledge and skills.
Limitations
The single-group pre–post design limits generalizability and precludes causal inference. The short intervention duration and notable attrition (119 to 66 matched responses) may have constrained detectable changes and introduced self-selection bias. Additionally, the questionnaire was not formally validated, underscoring the need for future research using rigorously developed and validated instruments.25
Conclusion
This study demonstrated that a practice-first Kolb experiential sequence is feasible in anatomy education and can produce a meaningful shift in students’ educational model preferences within a short period. The findings highlight the critical role of behavioral factors such as weekly study hours and preparedness in shaping this pedagogical adaptation. The absence of a short-term improvement in self-efficacy suggests that longer and repeated learning cycles may be required to strengthen this construct. Future studies should incorporate randomized controlled designs and objective outcome measures to assess the long-term impact of sequencing and its effects across diverse student populations.
Declarations
Ethics Declarations
All procedures performed in this study were conducted in accordance with the ethical standards of the institutional research committee and the principles of the Declaration of Helsinki. The study involved voluntary participation of medical students and did not include patient data or identifiable personal information. Data confidentiality and anonymity were strictly maintained throughout the study.
Animal and Human Rights Statement
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Electronic informed consent was obtained from all participants prior to inclusion in the study.
Data Availability
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Conflict of Interest
The authors declare that they have no competing interests.
Funding
None.
Author Contributions (CRediT Taxonomy)
Conceptualization: F.T.K.
Methodology: F.T.K., A.N.B.Y.
Formal Analysis: F.T.K.
Investigation: F.T.K.
Data Curation: F.T.K.
Writing – Original Draft Preparation: F.T.K.
Writing – Review & Editing: A.N.B.Y., B.K., B.N.Ç.G.
Supervision: A.N.B.Y.
Scientific Responsibility Statement
The authors declare that they are responsible for the article’s scientific content, including study design, data collection, analysis and interpretation, writing, and some of the main line, or all of the preparation and scientific review of the contents, and approval of the final version of the article.
AI Usage Disclosure
No artificial intelligence tools were used in the preparation of this manuscript.
Abbreviations
CI: Confidence Interval
CLT: Cognitive Load Theory
MD-PhD: Doctor of Medicine – Doctor of Philosophy
OR: Odds Ratio
PBL: Problem-Based Learning
SD: Standard Deviation
SPSS: Statistical Package for the Social Sciences
STROBE: Strengthening the Reporting of Observational Studies in Epidemiology
References
-
Gonsalvez DG, Ovens M, Ivanusic J. Does attendance at anatomy practical classes correlate with assessment outcome? A retrospective study of a large cohort of undergraduate anatomy students. BMC Med Educ. 2015;15:231. doi:10.1186/s12909-015-0515-y
-
Sbayeh A, Choo MAQ, Quane KA, et al. Relevance of anatomy to medical education and clinical practice: perspectives of medical students, clinicians, and educators. Perspect Med Educ. 2016;5(6):338-346. doi:10.1007/s40037-016-0310-4
-
Shtepura A. The impact of digital technology on digital natives’ learning: American outlook. Comp Prof Pedagog. 2018;8(2):128-133. doi:10.2478/rpp-2018-0029
-
Palla J, Moparthi S, Kaki S, Komaram R. Application of flipped classroom combined with problem-based learning: an effective learning approach to upgrade learning in medical students: a randomized controlled trial. MRIMS J Health Sci. 2023;12(1):13-19.
-
Nugroho D, Hermasari BK. Using online flipped classroom in problem-based learning medical curriculum: a mixed method study. J Educ Learn. 2023;17(2):294-300. doi:10.11591/edulearn.v17i2.20729
-
Kolb DA. Experiential learning: experience as the source of learning and development. 2nd ed. Upper Saddle River, NJ: Pearson Education; 2014.
-
Choshi M. Addressing challenges in undergraduate community health nursing clinical: Kolb's experiential learning theory. J Nurs Educ. 2025;64(6):e31-e34. doi:10.3928/01484834-20240513-02
-
Wang L, Du B, Fang D, Gao Y, Liu LW. Flipped classroom assisted by Rain Classroom for anatomy practical classes: challenges and opportunities of anatomy education. Anat Sci Educ. 2023;17(2):297-306. doi:10.1002/ase.2348
-
Wijnen-Meijer M, Brandhuber T, Schneider A, Berberat PO. Implementing Kolb’s experiential learning cycle by linking real experience, case-based discussion and simulation. J Med Educ Curric Dev. 2022;9:23821205221091511. doi:10.1177/23821205221091511
-
Yardley S, Teunissen PW, Dornan T. Experiential learning: transforming theory into practice. Med Teach. 2012;34(2):161-164. doi:10.3109/0142159X.2012.643264
-
Bentley DC, Pang SC. Yoga asanas as an effective form of experiential learning when teaching musculoskeletal anatomy of the lower limb. Anat Sci Educ. 2012;5(5):281-286. doi:10.1002/ase.1282
-
Lazari EC, Mylonas CC, Thomopoulou GE, et al. Experiential student study groups: perspectives on medical education in the post-COVID-19 period. BMC Med Educ. 2023;23(1):42. doi:10.1186/s12909-023-04006-9
-
Sweller J. Cognitive load during problem solving: effects on learning. Cogn Sci. 1988;12(2):257-285. doi:10.1207/s15516709cog1202_4
-
Hadie SNH, Sulong HAM, Hassan A, Ismail ZIM, Talip SB, Rahim AFA. Creating an engaging and stimulating anatomy lecture environment using the cognitive load theory-based lecture model: students’ experiences. J Taibah Univ Med Sci. 2018;13(2):162-172. doi:10.1016/j.jtumed.2017.11.001
-
Jamniczky HA, Cotton D, Paget M, et al. Cognitive load imposed by ultrasound-facilitated teaching does not adversely affect gross anatomy learning outcomes. Anat Sci Educ. 2016;10(2):144-151.
-
Naik BN, Rao R, Verma M, et al. Time management and readiness for self-directed learning among medical undergraduates of a tertiary healthcare institution: a cross-sectional study from Eastern India. J Educ Health Promot. 2025;14:53. doi:10.4103/jehp.jehp_407_24
-
Fleagle TR, Borcherding N, Harris JL, Hoffmann DS. Application of flipped classroom pedagogy to the human gross anatomy laboratory: student preferences and learning outcomes. Anat Sci Educ. 2017;11(4):385-396.
-
Wu H, Li S, Zheng J, Guo J. Medical students’ motivation and academic performance: the mediating roles of self-efficacy and learning engagement. Med Educ Online. 2020;25(1):1742964. doi:10.1080/10872981.2020.1742964
-
Abdulrahman KAB, Khalaf AM, Abbas FBB, Alanazi OT. Study habits of highly effective medical students. Adv Med Educ Pract. 2021;12:627-633.
-
Schweizer K. On the changing role of Cronbach’s alpha in the evaluation of the quality of a measure. Eur J Psychol Assess. 2011;27(3):143-144. doi:10.1027/1015-5759/a000069
-
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77-101. doi:10.1191/1478088706qp063oa
-
Sarkar S, Verma R, Singh S. Faculty and students’ perceptions on experiential learning based anatomy dissection hall sessions for medical undergraduates. Adv Med Educ Pract. 2022;13:543-554. doi:10.2147/AMEP.S359140
-
Friel K, Shultz ST. Anatomic donor surgeries increase self-efficacy in physical therapy education: use of live versus recorded viewing. Anat Sci Educ. 2023;16(6):1058-1072. doi:10.1002/ase.2315
-
Burgoon JM, Meece JL, Granger NA. Self-efficacy’s influence on student academic achievement in the medical anatomy curriculum. Anat Sci Educ. 2012;5(5):249-255. doi:10.1002/ase.1283
-
Boateng GO, Neilands TB, Frongillo EA, Melgar-Quiñonez H, Young SL. Best practices for developing and validating scales for health, social, and behavioral research: a primer. Front Public Health. 2018;6:149. doi:10.3389/fpubh.2018.00149
Figures
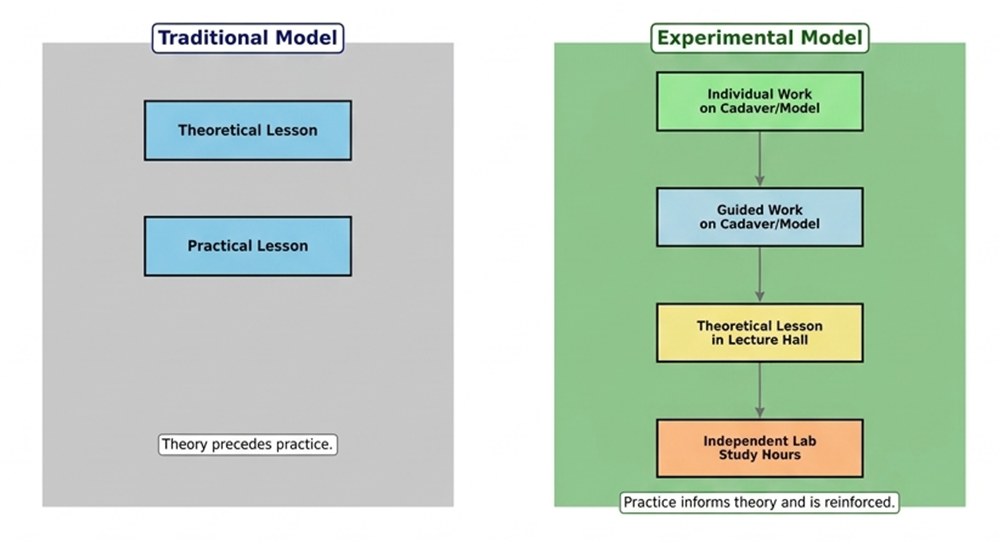
Figure 1. Comparison of traditional (didactic first) vs experimental (practice-first) sequence - schematic overview
This figure illustrates the differences between traditional (didactic preceding practice) and experimental (practice preceding didactic) models. The experimental model incorporates individual and guided work with cadavers/models, followed by didactic lessons and independent study hours to reinforce theoretical understanding.
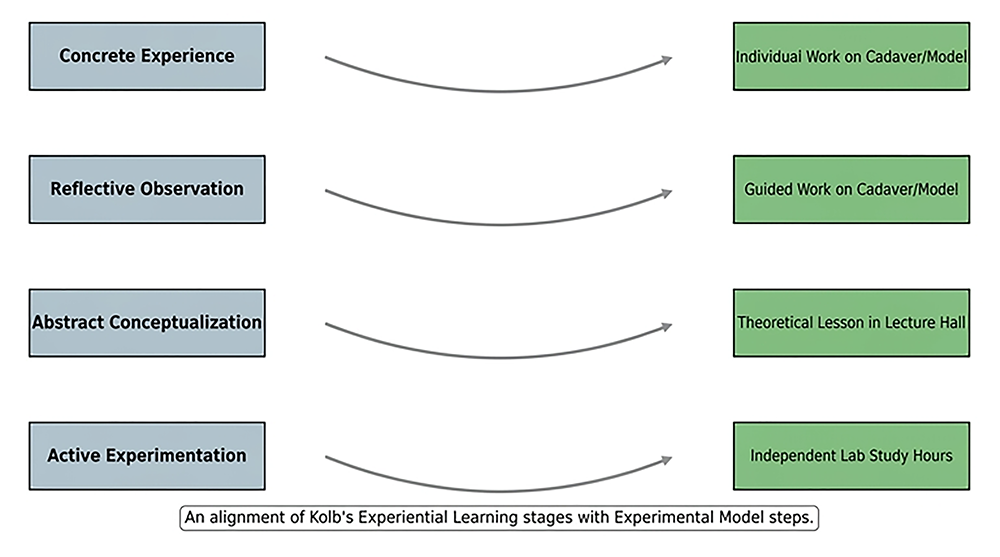
Figure 2. Enhanced comparison: Kolb’s experiential learning model vs. experimental model
This figure illustrates the alignment of Kolb's experiential learning stages (Concrete Experience, Reflective Observation, Abstract Conceptualization, Active Experimentation) with the corresponding steps of the experimental model implemented in this study (Individual Work on Cadaver/Model, Guided Work on Cadaver/Model, Theoretical Lesson in Lecture Hall, Independent Lab Study Hours).
Tables
Table 1. Demographic characteristics of participants (pre- and post-intervention surveys)
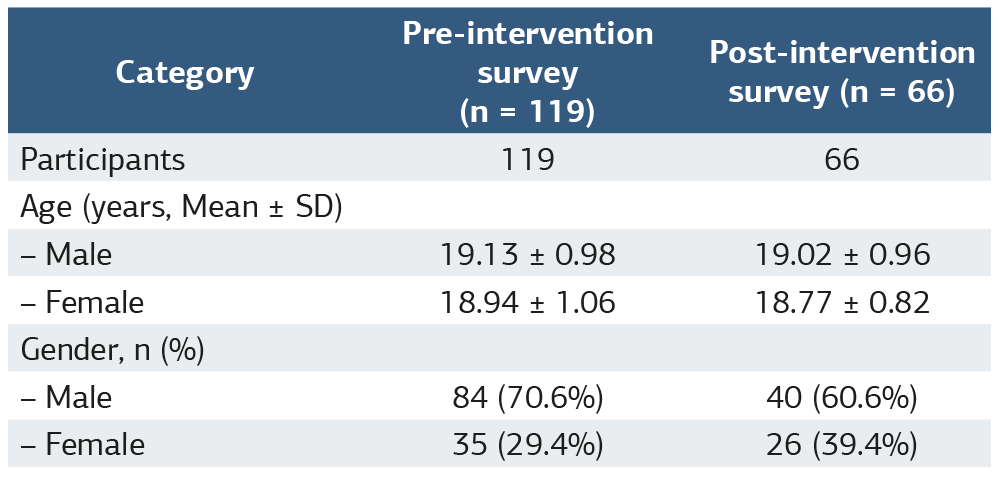
The table presents the mean age (Mean ± SD) and gender distribution of participants across the pre- intervention survey (N = 119) and post- intervention survey (N = 66) phases. Abbreviation: SD = Standart Deviation.
Table 2. Changes in educational model preferences between pre- and post-intervention surveys
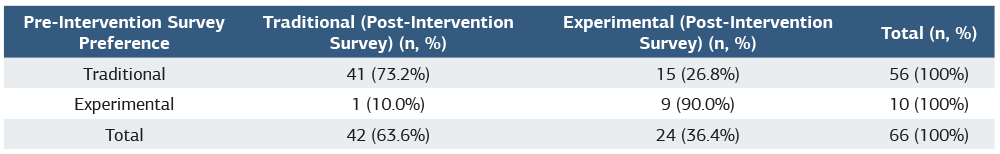
McNemar test results show significant shifts in preference toward the experimental model (p = 0.001).
Additional Information
Publisher’s Note
Bayrakol MP remains neutral with regard to jurisdictional and institutional claims.
Rights and Permissions
About This Article
How to Cite This Article
Reversing the traditional sequence in anatomy education: a practice-first experiential learning study. Ann Clin Anal Med 2026;17(Suppl 2):S181-186. doi: 10.4328/ACAM.50091
- Received:
- February 19, 2026
- Accepted:
- March 17, 2026
- Published Online:
- March 17, 2026
- Printed:
- March 20, 2026

